 I’ve had allergies for the past 49 years. Seriously. Started when I was two years old.
I’ve had allergies for the past 49 years. Seriously. Started when I was two years old.
My big problem is congested sinuses and nose. Loud breathing at night – drives my wife crazy just as it probably drove my folks crazy in the 60s. Sneezing over and over and over until I think my eyeballs are going to pop out and fly across the yard and land in the bird bath.
Perhaps you can relate.
I was recently going through a box of old stuff from my childhood (my Mom was good at keeping records, I guess). I uncovered a gem of a letter from my pediatrician from when I was not yet three years old. Literally typed out probably on an old IBM Selectric in courier font. I remember the smell of his office in that donut-shaped building by Southdale in Edina. Proof-positive that I have been suffering from allergies since the winter of 1966. To bolster my street cred on this, I’ve included as Exhibit A that very letter that for some reason my Mom kept all these years.

Thanks for your outpouring of sympathy.
Ah, spring!
The first robin on the grass. A gentle breeze blowing through the newly-budding trees. The rhododendrons are in bloom (the one in the picture above is from my front yard and could well be the source of all my nasal anguish). The birds are sweetly singing.
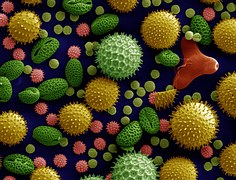
Pollen – magnified! (Public domain image)
And you can practically see the pollen floating through the air. Or at least your nose and eyes know it is there. Sneezy, itchy, watery, stuffy, headache-y. Such are allergies.
So what to do about seasonal allergies? I’ll get into all the sneezy details below, but first let me tell you about an exciting event and a friend of mine . . .
Announcing a live Twitter event: Allergy Hour!
Here at Healthy Matters production facilities (basically a room at HCMC, my hospital home) we are always looking for new ways to spread solid and fun medical info. The radio show started it all off (listen to Healthy Matters live on Sunday morning at 7:30 Central time on WCCO 830 AM or stream it live at WCCO.COM). Podcasts followed. Then we moved into blogs like this one and Twitter feeds (follow me @DrDavidHilden).
Now we are doing a special event called Allergy Hour from noon-1:00 on Wednesday, April 27.
Here’s how it works. During the hour, you simply send a tweet with your allergy question with the hashtag #allergyhour and we will answer it live via Twitter on my feed @DrDavidHilden. Simple as that. Sort of a rapid-fire, quick answer session to give you tidbits of information. Can’t wait to try it out – so put it on your schedule!
Dr. John B. Sweet
To help out with Allergy Hour, I’ve twisted the arm of my good friend Dr. John Sweet. Those of you who listen regularly to Healthy Matters on the radio or podcast (you know who you are and I thank you!) may know John. He is perhaps my most frequent guest as allergy topics are big big big for listeners.
Let me tell you about how I met Dr. Sweet. I met John B. Sweet (yes, indeed, his middle initial is “B” making the name ever-so-adorable, don’t you think) on the very first day of medical school. I was sitting with two other new classmates whom I had met about 5 minutes earlier. John joined Kara and Jennifer and me as the four of us had something in common; we were all starting medical school as a second career and were what were called “non-traditional” students by the youngsters in the class who were fresh out of college.
Johnny B was the studious one. Jen was wicked smart. Kara was wise and outspoken. I just talked during class a lot and distracted the three of them.
Who would have thought the four of us oddballs would become an outstanding allergist (John), family doctor (Kara), and dermatologist (Jen). Marriages and kids and careers and all that and we’re all still friends and hang out together. Awww.
Pardon that little diversion down memory lane . . . I just meant to introduce you to John, the allergist, but I got carried away in a bit of nostalgia.
So check out Allergy Hour! Wednesday April 27, noon-1:00, Twitter @DrDavidHilden and use the hashtag #allergyhour.
OK, now on to the hard-cord science.
Seasonal allergies 101
The basic situation with allergies is that your immune system is reacting, perhaps over-reacting, to a substance entering your body. Anything that causes such a reaction is called an allergen. There are a bazillion potential allergens that enter your body through many routes: ingestion (foods), skin (bee stings), nose & mouth (pollen and dust). I’m focusing on the last one – the seasonal allergies that come with simple breathing.
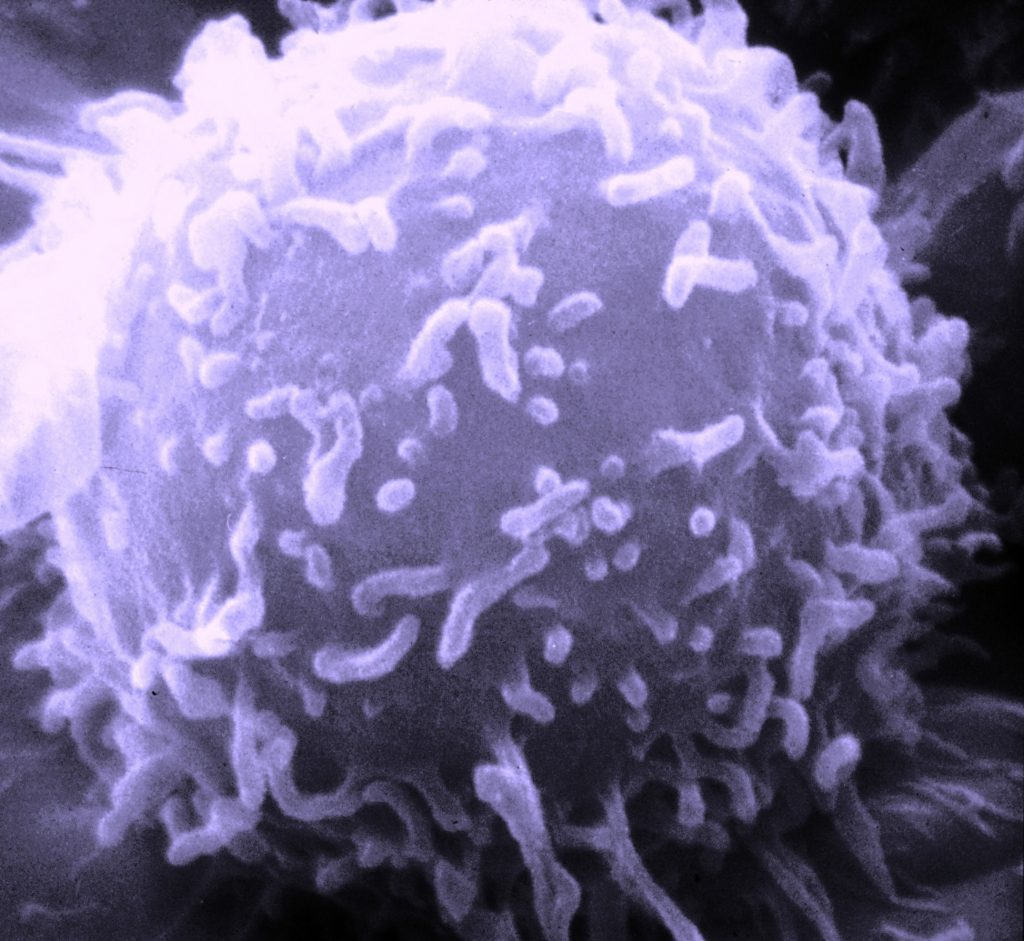
A lymphocyte, up close and personal (public domain image)
Before you over-react to your immune system’s over-reaction, it is good to remember that you really, really need that immune system. It is working to protect you, 24/7, from alien invaders to your body that are hell-bent on nefarious deeds, like getting you sick. Check out your friend the B lymphocyte in the incredible image at the left.
But for some of us, our immune system is a bit too exuberant. In the case of seasonal allergies, your immune cells see those little pollen specks or spores or dust particles and they go all out in waging battle. Like a general ordering the defense of the fort, they signal other cells – eosinophils, basophils, mast cells, and lots of others – to take up arms against the invaders.
Let’s take the army-guarding-the-fort metaphor probably a bit too far:
Command and control
Sentries: B lymphocytes
Always on the lookout for invaders, the B cells are a type of white blood cell who first encounter an invader (say, a pollen molecule that you just breathed in). Their job is to mobilize the troops to turn back the invaders. They do this by releasing antibodies. You might say they are the sentries – the watchdogs – of your body.
Spies and messengers: Antibodies
After being released under orders from the B cells, the antibodies, usually of a type called IgE or IgG (the Ig meaning “immunoglobulin”) fan out through the blood stream. Sort of like Paul Revere alerting the colonists.
Colonels: basophils, mast cells, eosinohils and others.
The messenger antibodies are picked up by these other white cells, each with a specialty purpose. They are the front lines of battle. Each a colonel with a job to do. Once they get the message from the antibodies, these white cells release inflammatory substances – things with names like cytokines, interleukins, histamine (recognize that last one?).
Infantry: cytokines
We’ll call these inflammatory proteins the infantry sent out to do battle. They lead to inflammation – a search-and-destroy mission intended to do away with the allergen invaders.
All this is necessary and good . . . to a certain degree. What if the inflammatory substances get out of hand? This is all happening in your tiny blood vessels in the linings of your body – the mucosal surfaces. These are areas like your sinsuses, nasal passages, mouth, airways. Inflammation = fluid and swelling. So you have a runny nose and you sneeze and your eyes itch. Misery ensues.
What to do . . . what to do . . . what to do?
Fortunately there is some relief. Anti-histamines are really quite effective. That is if you take them. As my wife will attest, I’m terrible at regularly taking my allergy meds. Best if you take it every day during the allergy season. The newer generation of anti-histamines (actually they are not that new) like loratadine, fexofenadine, and cetirizine don’t cause drowsiness in most people and only have to be taken once a day. Easy.
Here’s a cool site to check out the pollen counts where you live.
Note I’m using generic names here. I think that is a good practice to follow – whenever I can I try to use generic medications and names. You can find out the brand names if you want but you don’t have to spend the extra $$$ on the name brands. Generics will do just fine!
Other tips on reducing allergy symptoms:
- Close windows in your home, especially the bedroom. I hate this one since I really like sleeping with the window open. But it will probably help if you are allergic to something floating in the outside air.
- Get rid of rugs, carpets, curtains. Allergens just love to set up shop in these.
- Keep your place dusted. Yup, you gotta vacuum.
- Get tested for your specific allergens. Maybe you are allergic to tree pollen. Or grass. Or ragweed. These are all possible throughout the spring, summer, and fall, but most are more prevalent at one time or the other. During the higher pollen days, maybe avoid long outdoor exposure.

Ragweed
- Consider a topical nasal spray. These are anti-inflammatory in nature – remember the end-result of your allergy reaction is inflammation – so they may help a bit. Requires a prescription though.
- See your doctor about lots of other options. And I really do recommend seeing an Allergist like Dr. Sweet. These specialists have lots of arrows in their quiver to help out. And they can do skin testing and best of all – they can provide immunotherapy (allergy shots). The shots work by de-sensitizing your immune system so that over time your body won’t react so ferociously to minor allergens. Here’s a bit more about allergy shots.
You can learn lots more about allergies from the folks (who seem to have a thing for the letter “A”) at the American Academy of Asthma, Allergy, and Immunology. They are at aaaai.org.
That’s all for now.
One last entirely unrelated comment . . . you may have noticed the purple headings in this post. This week the world lost a bit of musical magic when Prince died. He grew up right near me in Minneapolis and though I never had a “Prince sighting” like so many others, his music was the music of my teenage years.
Rest in Peace, Prince.

